July 2012
By Polly Clayden and Mark Harrington
In nine countries, we enrolled 1763 couples in which one partner was HIV-1–positive and the other was HIV-1–negative; 54% of the subjects were from Africa, and 50% of infected partners were men. HIV-1–infected subjects with CD4 counts between 350 and 550 cells per cubic millimeter were randomly assigned in a 1:1 ratio to receive antiretroviral therapy either immediately (early therapy) or after a decline in the CD4 count or the onset of HIV-1–related symptoms (delayed therapy). The primary prevention end point was linked HIV-1 transmission in HIV-1–negative partners. The primary clinical end point was the earliest occurrence of pulmonary tuberculosis, severe bacterial infection, a World Health Organization stage 4 event, or death….As of February 21, 2011, a total of 39 HIV-1 transmissions were observed (incidence rate, 1.2 per 100 person-years; 95% confidence interval [CI], 0.9 to 1.7); of these, 28 were virologically linked to the infected partner (incidence rate, 0.9 per 100 person-years, 95% CI, 0.6 to 1.3). Of the 28 linked transmissions, only 1 occurred in the early-therapy group (hazard ratio, 0.04; 95% CI, 0.01 to 0.27; P<0.001). Subjects receiving early therapy had fewer treatment end points (hazard ratio, 0.59; 95% CI, 0.40 to 0.88; P=0.01). The early initiation of antiretroviral therapy reduced rates of sexual transmission of HIV-1 and clinical events, indicating both personal and public health benefits from such therapy.
—MS Cohen et al.[1]
The fact that treatment of HIV-infected adults is also prevention gives us the wherewithal, even in the absence of an effective vaccine, to begin to control and ultimately end the AIDS pandemic….For the first time in the history of HIV/AIDS, controlling and ending the pandemic are feasible; however, a truly global commitment…is essential. Major investments in implementation now will save even greater expenditures in the future; and in the meantime, countless lives can be saved.
—AS Fauci[2]
The yearly cost of achievement of universal access to HIV prevention, treatment, care, and support by 2015 is estimated at no less than US$22 billion. Implementation of the new investment framework would avert 12.2 million new HIV infections and 7.4 million deaths from AIDS between 2011 and 2020 compared with continuation of present approaches, and result in 29.4 million life-years gained. The framework is cost effective at $1060 per life-year gained, and the additional investment proposed would be largely offset from savings in treatment costs alone.
—B Schwartländer et al.[3]
INTRODUCTION
Three papers published in the past year[4],[5],[6] provide the scientific, public health, and policy framework for accelerating the response to the HIV pandemic such that within a few years the spread of HIV can be reversed, saving millions of lives and billions of dollars, using existing antiretroviral therapy (ART) introduced earlier and more broadly around the world. The only thing holding us back is the lack of economic and political leadership at the highest levels.
Juxtaposed against a background of economic distress and political paralysis in the world’s rich countries not seen since the early 1930s, the abundance of promising advances documented in this year’s i-Base/TAG 2012 Pipeline Report may seen unattainably out of reach to many of the millions of people who need them most. It will be the task of the activists, implementers, policy makers, and scientists attending this year’s International AIDS Conference in Washington, D.C., to work together to turn the tide so that everyone who needs high-quality treatment and prevention interventions for the global HIV, hepatitis C virus (HCV), and tuberculosis (TB) pandemics receives them.
Since the results of HPTN 052 were released last year,[7] HIV prevention and treatment research have moved ever forward; the interventions that have saved over 7 million people’s lives since the advent of highly active antiretroviral therapy (HAART) in 1996 are also proving to be remarkably powerful as HIV prevention measures. The HPTN 052 study set a very high bar for performance, as the measured 96% reduction in HIV transmission was built upon a high-quality clinical trial design and implementation, good prevention practice in both arms, and evidently very high adherence rates.
Although with less dramatic effect than HPTN 052, results of CAPRISA 004[8] (which used tenofovir as a topical vaginal microbicide, like some other preexposure prophylaxis [PrEP] studies such as iPrEx[9] which were released in the past two years, show that antiretrovirals can also offer protection when used by an HIV-negative partner, although the optimal use of these interventions is as yet uncertain. Table 1 shows the hierarchy of effect from clinical trial evidence using antiretrovirals for preventing sexual HIV transmission. But with all these studies, it is clear that adherence is required for treatment-as-prevention to work. Similarly, early studies in the HAART era showed that over 90% adherence was required for durable virological suppression among those taking treatment as treatment.
TABLE 1. Clinical Trial Evidence Using Antiretrovirals for Preventing HIV Infection
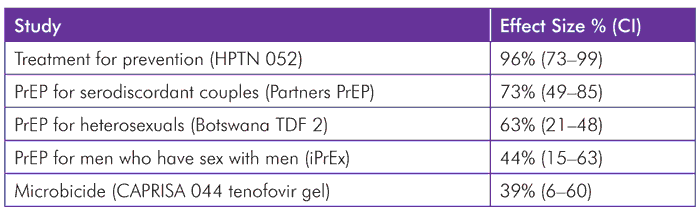
Source: Abdool Karim SS. CAPRISA 004 two years on: ten key lessons and their implications. Keynote address presented at: 2012 International Microbicides Conference; 2012 April 15; Sydney, Australia.
The potential contribution of these new discoveries to reduce the spread of HIV is directly threatened by today’s interlinked political and economic crises. Although a few administrative areas, such as the Canadian province of British Columbia and the city of San Francisco, California, have begun to provide universal offers of HIV treatment to all those referred to care, no country has yet started to fully implement these new interventions. The U.S. federal HIV treatment guidelines panel updated its recommendations in spring 2012 to recommend the universal offer of antiretroviral therapy (ART) to those with CD4 counts over 500 cells/mm3,[10] but it is too soon to assess whether this change is affecting practice in the United States. The panel’s recommendation is based on disease stage, and its statement of the primary (therapeutic) and secondary (preventive) benefits of ART, and the evidence base for this recommendation is worth reading in full:
The primary goal of antiretroviral therapy (ART) is to reduce HIV-associated morbidity and mortality. This goal is best accomplished by using effective ART to maximally inhibit HIV replication, as defined by achieving and maintaining plasma HIV RNA (viral load) below levels detectable by commercially available assays. Durable viral suppression improves immune function and quality of life, lowers the risk of both AIDS-defining and non-AIDS-defining complications, and prolongs life. Based on emerging evidence, additional benefits of ART include a reduction in HIV-associated inflammation and possibly its associated complications.
The results of a randomized controlled trial and several observational cohort studies demonstrated that ART can reduce transmission of HIV. Therefore, a secondary goal of ART is to reduce an HIV-infected individual’s risk of transmitting the virus to others. Although the Panel concurs that this public health benefit of ART is significant, Panel recommendations on when to initiate ART are based primarily on the benefit of treatment to the HIV-infected individual.
The strength of Panel recommendations depends on disease stage. Randomized controlled trials provide definitive evidence supporting the benefit of ART in patients with CD4 counts <350 cells/mm3. Results from multiple observational cohort studies demonstrate benefits of ART in reducing AIDS- and non-AIDS-associated morbidity and mortality in patients with CD4 counts ranging from 350 to 500 cells/mm3. The Panel therefore recommends ART for patients with CD4 counts =500 cells/mm3 (AI for CD4 count <350 cells/mm3 and AII for CD4 count 350 to 500 cells/mm3).
The recommendation to initiate therapy at CD4 count >500 cells/mm3 (BIII) is based on growing awareness that untreated HIV infection or uncontrolled viremia may be associated with development of many non-AIDS-defining diseases, including cardiovascular disease (CVD), kidney disease, liver disease, neurologic complications, and malignancy; availability of ART regimens that are more effective, more convenient, and better tolerated than earlier ART combinations no longer widely used; and evidence from one observational cohort study that showed survival benefit in patients who started ART when their CD4 counts were >500 cells/mm3.
Tempering the enthusiasm to treat all patients regardless of CD4 count is the absence of randomized data that definitively demonstrate a clear benefit of ART in patients with CD4 count >500 cells/mm3 and mixed results on the benefits of early ART from observational cohort studies. In addition, potential risks of short- or long-term drug-related complications and nonadherence to long-term therapy in asymptomatic patients may offset possible benefits of earlier initiation of therapy. When resources are not available to initiate ART in all patients, treatment should be prioritized for patients with the lowest CD4 counts and those with the following clinical conditions: pregnancy, history of an AIDS-defining illness, HIV-associated nephropathy (HIVAN), or HIV/hepatitis B virus (HBV) coinfection.[11]
In any case, with over two thousand Americans in nine states currently on AIDS Drug Assistance Program (ADAP) waiting lists,[12] the availability of HIV treatment as treatment for all HIV-positive residents of the United States is far from universal. It is unlikely that the preventive benefits of HIV treatment can be fully obtained until HIV treatment as treatment is available for everyone.
Last month’s unexpected U.S. Supreme Court decision to uphold the Affordable Care Act (ACA) provides a strong foundation for expanding HIV—as well as HCV—treatment, care, and prevention through the expansion of health coverage through both private insurance and public-sector Medicaid expansion. Over the next year, activists, policy makers, and researchers must build the foundation for the ACA and its accompanying health care expansion to underwrite the provision of universal voluntary treatment on demand for all people in the United States living with HIV and/or HCV infection.
Globally, the situation is grimmer. The past year saw the cancellation of the 11th round of funding by the Global Fund to Fight AIDS, Tuberculosis and Malaria (GFATM), the forced resignation of its highly respected executive director, pioneering AIDS researcher and activist Dr. Michel Kazatchine, his replacement by an unemployed Colombian banker named Gabriel Jaramillo, and the subsequent firing of many of the Global Fund’s staff. It’s not clear who has pulling the strings in this badly conducted Global Fund restructuring, but it is clear that the result has been a significant retardation of its programming. In the meantime, President Obama’s 2013 budget proposes to cut $550 million from the President’s Emergency Plan for AIDS Relief (PEPFAR), with a potentially dire impact on millions of people who are benefiting from PEPFAR programs.
We have been documenting President Obama’s disappointing record on AIDS since 2009.[13],[14] More recently, his administration’s lack of support for PEPFAR[15] threatens to undermine its impending legislative reauthorization, due in 2013.
Support for global HIV and tuberculosis (TB) programs from European countries such as France, Ireland, the Netherlands, and the United Kingdom, which have been significant donors to global health over the past decade, have been undermined during the past four years of economic turbulence. Meanwhile, the European Union (EU) superpower Germany, which has been a global-health deadbeat over the past decade, is now turning the screws on its own EU Mediterranean members, with predictably grim results for health: last year saw the first recrudescence of malaria in Greece since the disease was eliminated in 1974;[16] while in Athens, the cancellation of needle-exchange programs resulted in a whopping 1,250% increase in new HIV infections in the first 10 months of 2011 compared with the previous year.[17] (Astonishingly, late last year President Obama signed a reinstatement of the U.S. federal ban on needle-exchange funding as part of the 2011 budget deal with Congress.[18]) Seemingly everywhere in the so-called developed world, governments calculate politically and impose relentless economic austerity on their populations, regardless of the cost to health or lives. The consequences for their own citizens and for those who live in less developed nations will be high.
In some developing countries, however, domestic political will has coalesced around moving in a more positive and life-saving direction. After a titanic struggle going back to 1998, the Republic of South Africa initiated public-sector ART in 2003. More recently, following the departure of President Thabo Mbeki, whose regime and its institutionalized denial that HIV causes AIDS has been estimated to have led to at least 330,000 preventable deaths,[19] the current health minister, Dr. Aaron Motsoaledi, is administering an unprecedented rollout of HIV and TB testing and treatment with the goal of halving new HIV infections, achieving 80% HIV treatment coverage, and halving new TB infections and deaths by the year 2015.[20]
South Africa now has more people on HIV treatment than the United States has people living with HIV, and has the biggest ART program in the world. The country has made significant strides in reducing drug prices, decentralizing HIV care and treatment, and switching first-line therapy from stavudine; however, much more progress remains to be made in order to completely eliminate mother-to-child HIV transmission, treat pediatric HIV, and increase retention in care.[21] Moreover, the South African government is now paying for most of its HIV treatment program with domestic funds, replacing much of the scale-up support provided by PEPFAR and the Global Fund. However, this is unusual in most African countries or for that matter most developing ones.
All is not wine and roses in South Africa, however, as Nathan Geffen’s commentary below indicates, its National Strategic Plan has inspiring and aspirational goals, particularly compared with the Obama administration’s anemic National HIV/AIDS Strategy for the United States’ objectives to:
- lower new HIV infections by 25%;
- reduce HIV incidence by 30%;
- increase Americans’ knowledge of their own serostatus from 79% to 90%;
- increase the proportion of newly diagnosed patients linked to clinical care within three months of their HIV diagnosis from 65% to 85%;
- increase the proportion of Ryan White HIV/AIDS program clients who are in continuous care (at least two visits for routine HIV medical care in 12 months at least 3 months apart) from 73% to 80%;
- increase the percentage of Ryan White HIV/AIDS program clients with permanent housing from 82% to 86%; and
- increase the proportion of HIV-diagnosed gay and bisexual men, Blacks, and Latinos/Latinas with undetectable viral load by 20% each,
all by the end of 2015.[22]
The U.S. Centers for Disease Control and Prevention (CDC) estimates that between 48,000 and 56,000 Americans become infected with HIV each year.[23] Reducing this by the target of 25–30% would reduce new infections by 14,000–18,400 by the end of 2015, leaving 37,600–42,000 new infections each year by 2015.
The CDC estimates that only 28% of all Americans with HIV have an undetectable viral load.[24] Thus, increasing this by 20% in absolute terms would mean that 48% of HIV-positive Americans had an undetectable viral load by the end of 2015, leaving 52% of them with detectable HIV, and the risk of progression and onward transmission. (Another report suggests that just 19% of Americans with HIV have an undetectable viral load, which would result in coverage by 2015 being even lower.[25])
Even assuming the CDC’s estimate that 28% of HIV-positive Americans have an undetectable viral load, the status quo is unacceptable, and the full achievement of the National AIDS Strategy’s uninspiring goals will leave a huge cost to future generations in dollars, health, and lives.
Only an estimated 28% of all HIV-infected persons in the United States are virally suppressed, largely because even among those with diagnosed infection, only 51% are receiving regular HIV care. Without substantial improvement in these percentages, 1.2 million new HIV infections would be expected to occur in the United States over the next 20 years.[26] Based on estimated lifetime HIV treatment costs of $367,000 per person (2009 dollars)[27] caring for persons who become infected could cost as much as $450 billion in health-care expenditures.[28],[29]
One reason for the failure of the U.S. National AIDS Strategy to focus on more ambitious goals is the administration’s preemptive requirement that few to no additional resources be expended in the domestic fight against HIV. A recent publication indicates that without significant and immediate scale-up of HIV prevention, testing, and treatment, “key goals of the NHAS will soon be epidemiologically out of reach.”[30]
As noted above, however, the recent decision upholding the constitutionality of the ACA provides a framework for achieving universal voluntary treatment on demand in the United States for those with either or both HIV and HCV infection.
Needless to say, political will for the prevention and treatment of HCV and TB, despite their worldwide extent and deadly toll, is even weaker than it is for HIV.
Worldwide, TB rates are falling too slowly, while new infections with drug-resistant TB are on the increase almost everywhere. The current infrastructure for “controlling” TB is failing for people with HIV, children, and those with drug-resistant disease. While some progress is apparent in therapeutics and diagnostics development, these advances have yet to translate into sufficiently concrete reductions in incidence, disease, or death.
There are no domestic reimbursement programs for HCV treatment, and globally—despite the recent progress in Thailand described by Karyn Kaplan in her chapter below—neither a public health– nor an individualized medical approach to HCV prevention and treatment is in place. The promise of recent progress toward all-oral direct-acting antiviral (DAA) therapy will remain unfulfilled until infrastructure is created, in the United States and globally, to treat all those in need.
It is to be hoped that the activists, implementers, policy makers, and researchers who participate in the 2012 International AIDS Conference in Washington, D.C., will raise their voices to ensure that the United States adopts more ambitious goals both for its own domestic epidemic and for the global pandemic.
Below we review in brief the promising abundance of new prevention and treatment options for HIV, HCV, and TB, which are more fully detailed in the subsequent chapters.
EXECUTIVE SUMMARY
HIV
Simon Collins provides an incisive and comprehensive overview of the currently vibrant state of antiretroviral drug development. Last year saw the approval by the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA) of the new non-nucleoside reverse transcriptase inhibitor (NNRTI) rilpivirine (Janssen’s Edurant) and its inclusion in a fixed-drug combination (FDC) with Truvada (emtricitabine[FTC]/tenofovir) as Complera/Eviplera (Janssen/Gilead). This year is likely to see another new chemical entity and another FDC approved by the FDA and the EMA, in this case the second available integrase inhibitor, elvitegravir, alongside the first pharmacokinetic booster since ritonavir (and the first developed exclusively as a booster), cobicistat, co-formulated along with FTC/tenofovir disoproxil fumarate as Quad (Gilead).
Quad is noteworthy for being the first FDC to be submitted to regulatory authorities as a fixed-dose combination product before new drug applications for two of its individual components as single agents (i.e., elvitegravir and cobicistat) were submitted. Gilead filed Quad with the FDA on December 23, 2011, but it only filed for elvitegravir as a single drug on June 27, 2012 (and then for cobicistat the day after that). The FDA is expected to act on Quad by August 27, 2012.
As noted in table 2, a number of additional FDCs are in development from Gilead, Janssen, and ViiV Healthcare including those based on cobicistat-boosted darunavir, and the third integrase inhibitor, dolutegravir, both combined with two NtRTIs (nucleotide reverse transcriptase inhibitors).
Another noteworthy advance from 2011 is the rapid progress of GS-7340, the investigational tenofovir prodrug whose advantages include improved pharmacokinetics and cellular penetration, enabling it to be given at doses as low as 10–25 mg/day compared with the current formulation of tenofovir, tenofovir disoproxil fumarate (TDF), which is dosed at 300 mg/day.
Assuming the sponsor, Gilead, pursues tiered-pricing and voluntary licensing approaches it has followed to date, this drug provides the possibility of a much cheaper NtRTI that could replace TDF and be available at a much lower price threshold, at least in developing countries, further weakening the rationale for pursuing such desperate—and toxic—measures as 20 mg/day of stavudine.[31]
Activists and people with HIV have been protesting from South Africa[32] to India[33] against a study comparing 20 mg/day of stavudine with tenofovir, which is proposed to take place in Uganda, India, and South Africa, for at least five reasons:
- Stavudine’s long-term toxicity question at 20 mg will not be answered by this trial;
- Stavudine is more toxic than tenofovir at 30 mg. This is not expected to be sufficiently mitigated by dose reduction as the toxicities are dose- and time-dependent, and for this reason it is an inferior treatment option;
- The poor tolerability of stavudine limits therapeutic durability;
- Stavudine’s side effects detract from stavudine’s savings on cost; and
- Stavudine can compromise second-line options.
As we go to press, a detailed report on the study was just broadcast on e.tv news—the biggest television news program in South Africa—which would have been seen by millions of people. Patients with terrible lipoatrophy were interviewed and made it clear they want d4T phased out. Perhaps it is time to remind funders and researchers of the critical role of community mobilization espoused in the WHO and UNAIDS Treatment 2.0 Framework Initiative, which describes one of its goals as: “People living with HIV and key populations are fully involved in the demand creation, planning, delivery and evaluation of quality-assured, rights-based HIV care and treatment programmes in all lower/middle income countries.”[34] Along with treatment activists and people with HIV around the world, who know all too well the lifelong and sometimes crippling, stigmatizing toxicities of stavudine (d4T), the authors of this report hope that funders and investigators leading the proposed study turn their attention to more relevant and less retrograde approaches to treatment optimization.
Last year’s Pipeline Report described the past decade as a “golden age of antiretroviral drug development.”[35] Here we are happy to update that report’s table 1 showing the status of all antiretroviral compounds reported in TAG and i-Base pipeline reports since 2003 (see table 2, HIV Treatment Pipeline, 2003–2012, below), which shows that the success rate for new molecular entities (NMEs) and FDCs that were in phase II or beyond between 2003 and 2012—assuming imminent FDA/EMA approval for elvitegravir, cobicistat, and Quad—will be 18/63, or 28.6% (down slightly from last year’s reported 14/46 or 30.4%, due principally to the addition of new candidates rather than to increased attrition).
TABLE 2. HIV Treatment Pipeline 2003–2012
Click here to download a full size pdf of this table.
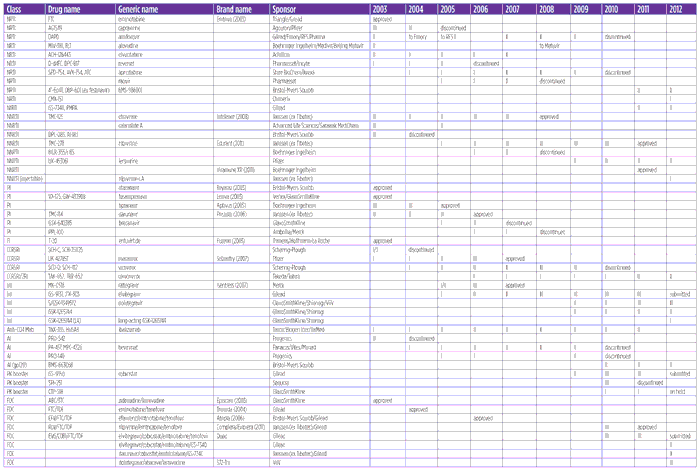
LEGEND: NRTI = nucleoside reverse transcriptase inhibitor; NNRTI = non-nucleoside RTI; PI = protease inhibitor; FI = fusion inhibitor; CCR5RI = CCR5 receptor inhibitor; CCR2RI = CCR2 receptor inhibitor; InI = integrase inhibitor; AI = attachment inhibitor; MI = maturation inhibitor; PK booster = pharmocokinetic booster; FDC = fixed-dose combination
In her synoptic update, Polly Clayden describes “a flurry of activity in pediatric antiretroviral drug development and approval,” but notes that “the short-and medium-term requirements of the youngest children in resource-limited settings still badly need to be addressed,” with “too many formulations and yet too few real options.” There are “over 45 single agents and co-formulations” but “the market is very small, and further fragmented by different regimens across age groups and weight-band doses.”
Notwithstanding this daunting complexity, the last year saw FDA approval of oral suspension formulations of darunavir for children ages 3–<5 and children >6 unable to swallow darunavir tablets; chewable raltegravir tablets for children 2–18 years old; oral powder and tablets of tenofovir for children 2–<18 years old; etravirine tablets for children 6–18 years old; and last—and probably of least significance, particularly in developing countries—an oral suspension of fosamprenavir for children 4 weeks to <6 years old.
It’s probably noteworthy that over the past year, the FDA has approved more drugs[36] for children than for adults.[37]
Of course, FDA approval alone is irrelevant to most of the world’s HIV-positive children, who live outside the United States. Clayden calls for all stakeholders to work together to expedite development of and access to the most useful, potent, and safe drugs and combinations for children of all ages. It is critical that we shorten the time from clinical trial successes in adults to those in children (and in turn throughout the age ranges), and then from FDA/EMA approval to availability of drugs where they are most needed.
On the HIV point-of-care diagnostics front for both CD4 cell quantification and viral-load testing, we find progress since last year to be so underwhelming—in spite of a spate of sponsors’ claims that this year would be an annus mirabilis of point-of-care diagnostic test validation, approval, and rollout – that we decided to include only last year’s CD4 point-of-care test pipeline, viral load point-of-care pipeline, and p24 test for EID (early infant diagnosis) pipeline (tables 3 to 5) with a few barely discernible tweaks.
TABLE 3. CD4 Point-of-Care Test Pipeline
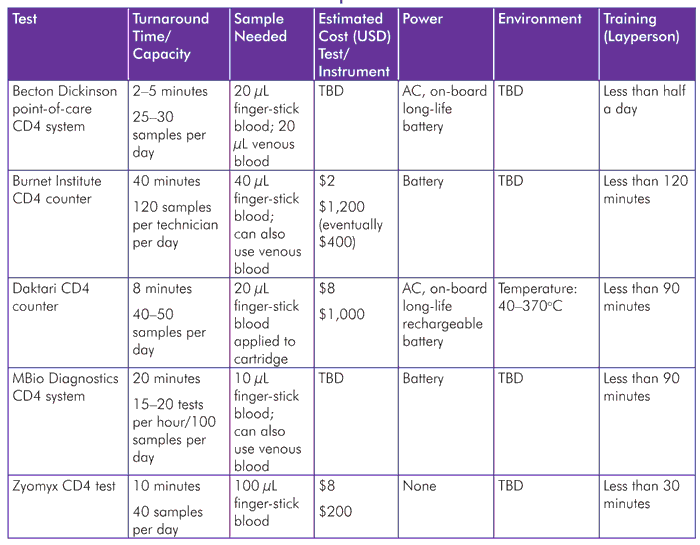
TABLE 4. Viral Load Point-of-Care Test Pipeline
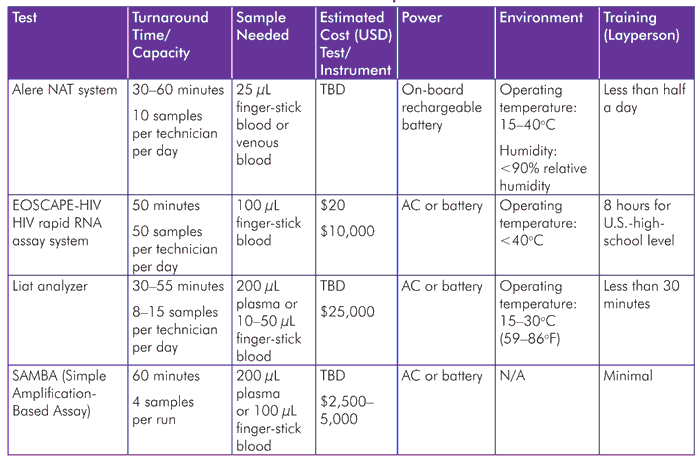
TABLE 5. p24 Test for Early Infant Diagnosis (EID)
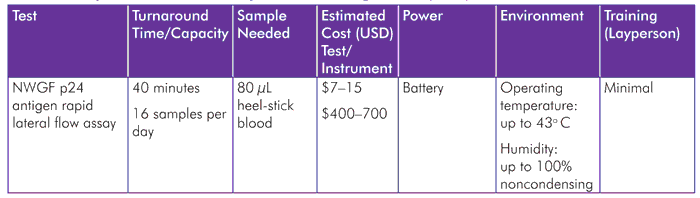
Source: Murtagh M. UNITAID HIV/AIDS.[38]
Of the four CD4 tests described last year, one (Daktari) expected commercial launch at the end of 2011, and another (Zyomyx) to be available this year.[39] Both are now commencing clinical trials this year. Burnet field trials were planned in Malawi for 2011 (now 2012 due to the change in the CD4 threshold for treatment initiation from 200 cells/mm3 to 350 cells/mm3). MBio continues field evaluations. The launch of a new test from Becton, Dickinson and Company (BD), using image-based counting technology, is currently expected in 2012.
Alere and Liat tests were also due to be launched in 2012 (now 2013) and still possible in 2012, respectively. SAMBA continues to be field tested with Médecins Sans Frontières (MSF). The new addition, EOSCAPE-HIV, predicts a launch in 2013.
Finally, the NWGHF p24 for EID has also bumped its predictions for clinical and field trials and launch from 2011 and 2012, to 2012 and 2013, respectively.
Meanwhile UNITAID has committed substantial new funding to implementation partners MSF and the Clinton Health Access Initiative (CHAI)[40] to establish best practices for the use of new point-of-care technologies in resource-limited settings (RLS) and to expedite access to these tests at the lowest possible price, respectively, so perhaps the predicted bumper year may not be too far away. We look forward to reporting a more bubbling pipeline next year.
Last year’s lack of progress in point-of-care tests allows us, however, to expand last year’s coverage of treatment optimization (see “Less of the Old—or More of the New?” 2011 Pipeline Report)[41] into its own chapter this year, “Retrofitting for Purpose.” Clayden provides a brisk overview of all the approved and pipeline drugs that are likely to play an important role in treatment optimization—which includes extending durability and potency, reducing toxicity to a minimum, enhancing tolerability, and reducing cost, ideally together—and concludes with three simple maxims, to wit:
- Treatment optimization must be in the interests of people with HIV;
- Drugs and regimens need to be designed with resource-limited settings in mind; and
- Shorten time between full FDA/EMA approval and WHO prequalification, and FDA tentative approval and that by local regulatory agencies.
Here Clayden brings out a key message, which is that the policy and regulatory pipeline linking FDA/EMA approval, WHO prequalification, FDA tentative approval, and approval by national regulatory authorities in high-burden countries (not to mention inclusion in local guidelines and timely generic products) is becoming an increasingly urgent issue not only for HIV but for TB and, soon, for HCV as well. Nathan Geffen provides a sobering update on this regulatory emergency from South Africa.
A Regulatory Reality Check from South Africa
By Nathan Geffen*
The approval of drugs by the FDA or EMA does not automatically translate into approval or access to these drugs in places with the greatest number of patients. Older drugs with worse side-effect profiles, like stavudine, didanosine, and zidovudine, are consequently still widely used throughout sub-Saharan Africa. Newer agents like raltegravir are barely used at all.
South Africa, which has good treatment data and statistics, as well as a full-fledged regulatory authority, the Medicines Control Council (MCC), provides useful examples.
Tenofovir was approved by the FDA in 2001. It was approved by the MCC only in 2007, and then only after public pressure including demonstrations against the MCC and the drug company responsible for registering it with the agency. Tenofovir only became recommended in South Africa for the first time in the Department of Health’s 2010 adult Antiretroviral Treatment Guidelines,[42] and was widely available in the public sector only after that. Consequently about half a million people still use stavudine as part of their first-line regimens in the South African public sector. New patients are prescribed tenofovir, lamivudine, and either nevirapine or efavirenz. However, stock-outs of tenofovir since late 2011 until the time of this writing in mid-2012 have resulted in the Southern African HIV Clinicians Society issuing the following guidance to health workers in case of shortages: “If a patient on [tenofovir] is virologically controlled and there is a TDF shortage…[t]he patient can be safely, in the short term, switched to d4T 30 mg bd [twice daily] or AZT 300 mg.”[43]
There have also been stock-outs of abacavir, a drug recommended in the pediatric guidelines. Recently, this may have been associated with the tenofovir stock-outs, i.e., adult patients had substitutions with abacavir, which in turn used up supplies intended for older children.
Despite the approval of several combination antiretroviral medicines and their availability at reasonable prices in the private sector, public-sector patients, with a few exceptions, are still dispensed single-drug pills. The monthly cost of a generic equivalent of Atripla in the private sector is about US$50. This compares to less than US$20 per month for tenofovir, lamivudine (as opposed to FTC), and efavirenz purchased separately on the public-sector tender. However, if more combination medicines were put out for bidding, their prices would likely compete with those of the three drugs bought separately.
For new agents, access is particularly unpromising. Raltegravir is available in the private sector at about US$110 per month. Etravirine is about US$100 per month. These products are unaffordable to all but a few South Africans. Private medical plans, except in a few limited cases, do not pay for these. They are unavailable for general use in the public sector. No generic versions are available. Atazanavir is not purchased on the public-sector tender, and its private-sector price is about US$12 per month more expensive than that of lopinavir/ritonavir. The private-sector price of darunavir, also not available on the public-sector tender, is more than double that of lopinavir/ritonavir, and there is only one supplier. Maraviroc is not listed in the private-sector drug list, and possibly not yet approved. (Unfortunately, the MCC does not keep an easily accessed public database of approved drugs, so this cannot be verified easily.) Rilpivirine is not approved yet. The price of fosamprenavir, at US$185 per month, renders it unaffordable to virtually everyone. But tipranavir is the most unaffordable antiretroviral, at over US$500 per patient per month in the private sector. (As far as I can tell, extended-release nevirapine is not yet available in South Africa.)[44],[45]
This means that second-line and salvage-regimen options are limited for public-sector patients. Department of Health guidelines still recommend didanosine for second-line treatment to children over three who were on abacavir, lamivudine, and efavirenz in their first-line regimen. Zidovudine is recommended in the second-line regimen for patients failing tenofovir-containing regimens.
The situation in South Africa is replicated, more or less—and often less—in most sub-Saharan African countries. There are several reasons why access to new agents in developing countries lags so far behind their approval by the FDA and EMA:
- Regulatory authorities, such as the MCC, are inefficient and weak. The MCC’s approval of fixed-dose combination antiretrovirals has been very slow.
- Drug companies do not prioritize getting their agents approved in developing countries, where profits are small.
- Stricter global patent protection means that generic versions of newer agents are either not available at all or their availability is very limited. Raltegravir, atazanavir, etravirine, rilpivirine, darunavir, and tipranavir are examples of this. The production processes of newer agents are often more expensive as well.
- Guidelines are infrequently updated, so new treatment advances are not taken advantage of.
- The South African Department of Health has been slow to adopt fixed-dose combination medicines despite generic production of first-line regimen combination products and their many advantages.
- Stavudine and didanosine are among the cheapest antiretrovirals, making them attractive to programs with more patients than they can afford to treat.
On the positive side, the relatively late start to antiretroviral treatment throughout Africa means that the vast majority of patients are still on first-line regimens. Tenofovir is becoming more widely available, and stavudine is slowly being phased out.
*Nathan Geffen is treasurer of the Treatment Action Campaign (TAC) and the author of Debunking Delusions: The Inside Story of the Treatment Action Campaign (Jacana Media, South Africa, 2010). We thank him for this contribution.
In his extensive, reflective, and unprecedentedly upbeat overview of the diverse pipelines made up of HIV preventive therapies, immune-based and gene therapies, and research toward a cure, Richard Jefferys documents the first filing for FDA approval of any intervention to prevent sexual transmission of HIV—in this case, Gilead’s filing a supplemental new drug application (SNDA) for Truvada (emtricitabine/tenofovir) to prevent HIV transmission in serodiscordant couples, among men who have sex with men, and for others at risk of sexual acquisition of HIV.
After an extensive national debate, and lopsided FDA Antiviral Drugs Advisory Committee recommendations for approval (19–3 for men who have sex with men [MSM], 19–2 for HIV-negative partners in serodiscordant couples, and 12–8 for others at risk), final FDA action is expected by September 14, 2012.
It remains unclear what FDA approval will mean in practice—though it usually leads to reimbursement by private insurers and Medicare—let alone what the implications are for RLS.
Additional studies of preexposure prophylaxis (PrEP)—including both vaginal and oral approaches—remain underway, with some novel compounds such as DAPY (formerly TMC120) entering clinical trials, as well as some drugs that have yet to find their niche, such as Pfizer/ViiV’s CCR5 receptor blocker maraviroc.
HIV vaccine researchers continue their dogged, thoughtful efforts to develop effective vaccine approaches, building on the apparent—but limited—success of the prime-boost approach used in RV144, and hoping to avoid the pitfalls of the STEP adenovirus-5-based vector system. The field remains a long way from a licensed product, but continued investment will be vital to the pandemic endgame.
HIV cure research continues to enjoy increased investment and attention. Last year, the National Institute of Allergy and Infectious Diseases (NIAID) awarded $70 million over five years to three Martin Delaney Collaboratories to carry out basic and clinical cure-related research.[46] The applications must have been good, because NIAID initially planned to commit only $42.5 million for these grants.
Following an international community-driven workshop in April 2011 on clinical research issues facing HIV cure-related research,[47] the U.S. FDA and National Institutes of Health (NIH) commissioned the Forum for Collaborative HIV Research to convene an 18-month public scientific and community-inclusive advisory process to coordinate and harmonize regulatory, scientific, community, and ethical approaches to HIV cure-related clinical trials.
This week will see the release, after two years of effort, of the International AIDS Society (IAS)-led global scientific strategy, Towards an HIV-1 Cure.
Achieving a globally scalable HIV cure will most likely require one or a combination of small molecules that can be taken orally over a period of weeks or months. A major difficulty in HIV cure research is measuring the HIV reservoir. Curing HIV means eliminating replication-competent HIV from the body. Current methods for detecting very low levels of HIV in the body are at the very limit of detection. It is possible that someone could be cured while still having cells that were infected with defective, non–replication competent HIV. In those cases, fragments of HIV DNA, -RNA, or proteins might still be detectable even if replicating HIV was absent from the body. It will be crucial to discover and develop better quantification tools to measure HIV at the very lowest levels of detection in order to confirm experimentally the results of cure-related clinical interventions.
Jefferys notes that few new cure-related approaches have entered the clinic since 2011.
Related research continues on cellular and gene-therapy approaches to HIV treatment as well as putative HIV therapeutic vaccines. Each of these approaches—or none—may ultimately be required to cure HIV infection from infected individuals.
HCV
The hepatitis C virus (HCV) is a virological latecomer, discovered only in 1989 (whereas TB was discovered in 1882, and HIV-1 in 1982). HCV is curable, unlike hepatitis B virus (HBV) or HIV. Until 2011, when the first two hepatitis C protease inhibitors were approved, the standard of care for HCV was pegylated interferon and ribavirin, which was poorly tolerated due to a constellation of neuropsychiatric, constitutional, and hematologic side effects, and was often ineffective. Adding a third drug has made HCV treatment more effective, but tolerability is suboptimal, and triple therapy is challenging to administer—and to endure. Fortunately, many oral drugs from different classes are in development to treat—and cure—HCV.
In this year’s Pipeline, Tracy Swan’s epic overview of the explosive therapy developments in HCV demonstrates the swift application of many of the paradigms developed for HIV in the 1990s – combination trials, real-time virological monitoring of therapy—to HCV, with extremely promising results. Some two- or three-drug combinations of all-oral DAAs against HCV have demonstrated an unprecedented ability to cure the disease in both treatment-naive and treatment-experienced people.
For the most part, DAA combination trials have enrolled people who are easily treated. Swan notes with disfavor that there are no data from people with cirrhosis, transplant candidates and recipients, and HIV/HCV-coinfected people. Unfortunately, DAAs may not reach people who are unable to wait until they are approved. Despite increasing pressure from activists, regulators, and desperate patients and their physicians, pharmaceutical companies have refused to provide early access to DAA combinations through open-label trials or other initiatives. A critical opportunity to collect information on drug safety and efficacy—and to offer potentially lifesaving treatment to people with urgent need—is being squandered.
We hope that as a result of Swan’s dauntless advocacy, current and future sponsors will take heed and expedite safe and efficient development of these new combination approaches in HIV-coinfected as well as HCV-monoinfected persons.
Swan notes that, domestically, the infrastructure and reimbursement mechanisms that will be needed to reach all the nation’s HCV-infected persons do not yet exist. This grim reality may blunt the rapid return on investment on which the HCV DAA combination therapy revolution is based.
Globally, there is no public-health approach even proposed for HCV prevention, diagnosis, and treatment, although at least 160 million people are chronically infected with this virus, and many will progress to end-stage liver disease unless they are treated and cured. To address this growing need, Karyn Kaplan’s chapter—focusing on HCV/HIV-coinfection treatment activism in Thailand—demonstrates how a group of HIV-positive treatment activists rooted in Thailand’s drug user community and linked with treatment activists from New York were able, after a long and challenging effort, to persuade the Thai government to begin including HCV treatment as part of its universal health care plan in 2012. TAG, i-Base, and our colleagues around the world hope that other developing countries move in this direction, and that the sponsors of innovator compounds to treat and cure HCV will be made available at appropriate tiered pricing levels through voluntary licenses—and if necessary through compulsory ones—so that everyone with chronic HCV infection has access to treatment over the coming decade.
TB
Though TB is the oldest of the three pathogens against which the products discussed in this report are aimed, efforts to control it globally—let alone to eliminate it as a public health threat by the year 2050 as the global Stop TB Partnership aims to do—are faltering.
Anti-TB work is hobbled by the lack of a cheap, accurate point-of-care diagnostic test that can detect within minutes, and without electricity, a cold chain, or sophisticated laboratory equipment, all the forms of this disease, which has been with humanity since before recorded history.
As Colleen Daniels and Coco Jervis show us in their depressing overview of TB diagnostics research, the pipeline for discovering such a point-of-care test for TB is a mere trickle, one in danger of drying up completely for lack of investment and long-term commitment. After a few years during which several improvements in TB culture- and molecular testing were developed, approved by the World Health Organization (WHO), and rolled out in developing countries, there has been a relative drought. Twice in the last two years, the WHO expert panel reviewed—but did not recommend for wide-scale use—a rapid molecular test to detect extensively drug resistant (XDR) TB.
In 2010, the WHO did recommend wide scale-up of the Cepheid GeneXpert MTB/RIF test, which can detect the presence of TB and resistance to two of the most commonly used drugs—isoniazid and rifampicin—within two hours. However, the test requires trained laboratory staff, electricity, annual calibration at a facility in Toulouse, France; and the machine costs US$17,000, while currently the price per cartridge is US$17—making it inaccessible to lower-income countries and barely affordable in middle-income countries such as South Africa where the burden of TB is high, and its extent hard to detect because of the high rate of HIV coinfection. Last month, the U.S. government (including USAID and the Office of the Global AIDS Coordinator/PEPFAR), along with UNITAID and the Bill & Melinda Gates Foundation, approved a proposal to accelerate and front-load purchases of the Xpert cartridges from Cepheid, which should allow the cost-per-cartridge to come down to US$9.98 as soon as this month. It remains to be seen whether this cost reduction is sufficient to allow the test’s deployment where it is most needed.
The last year saw notable advances in the TB treatment pipeline, as discussed in Erica Lessem’s elegant overview. These advances included results of the first novel combination regimen study for TB (the TB Alliance’s NC001 study of PA-824, moxifloxacin, and pyrazinamide, which is now going into a joint study in both drug-sensitive and drug-resistant TB); the first compassionate use program for a new TB drug ever (Janssen’s open-label compassionate use study of the diarylquinoline bedaquiline [formerly TMC207]); EMA filing of the first new TB drug and class since the 1970s (Otsuka’s delamanid, formerly OPC67683); peer-reviewed publication of the phase II Otsuka study in persons with drug-resistant TB; and the establishment by a global coalition of activists of the TB Community Advisory Board (TB CAB), which has met in Washington, D.C., and in Durban, South Africa, to increase community engagement with TB research.
Finally, earlier in July 2012, Janssen (formerly Tibotec) announced its FDA filing for accelerated approval for bedaquiline (formerly known as TMC207), for the treatment of drug-resistant TB.[48] We hope that EMA and FDA actions on delamanid and bedaquiline take place with an awareness of the urgent and expanding threat posed by drug-resistant TB worldwide.
For the first time, it is possible to envisage a future in which people with all forms of TB, whatever their resistance profile, could be treated with a curative regimen made up of drugs to which the infecting organism is susceptible. This would involve a combination of new and existing compounds, or all-new drugs—if the six novel agents currently in phases I–III, or their successors, are safe and effective enough for wide use. It is still far too early to be certain of success, and unlike with HCV or HIV, there are far too few innovator compounds—or companies—yet in the clinic. Recent indications from the FDA of potential regulatory flexibility regarding endpoints for registrational studies are encouraging.
As with HIV, the TB vaccine field remains less well populated with candidates or companies, but a safe and effective vaccine against pulmonary transmission of TB will remain a requirement if the disease is ever to be eliminated. Richard Jefferys notes in his chapter on TB vaccine development in 2012 that the pipeline is not growing as fast as it needs to.
On May 30–June 1 2012, a group of activists, implementers, policy makers, and researchers, met in Cambridge, Massachusetts, to focus on how to achieve the most rapid possible reduction in new TB infections, TB deaths, and suffering and stigma caused by TB. The statement by this group on “Zero New TB Infections, Zero TB Deaths, and Zero TB Suffering,” will be released this week in Washington, D.C.
