Selected updates to this chapter will be posted below prior to the 2013 edition of the Pipeline Report.
Feburary 2013 Update
Additional clinical trials in the Research Toward a Cure/Therapeutic Vaccines/Gene Therapies categories:
Safety Study of a Dual Anti-HIV Gene Transfer Construct to Treat HIV-1 Infection
July 16, 2012
The U.S. Food and Drug Administration has approved Truvada for the prevention of HIV infection in individuals at high risk of acquiring HIV through sexual exposure. See the FDA press release (which includes links to additional information resources), updated guidance documents from the U.S. Centers for Disease Control (CDC), and the AVAC PrEP page.
July 2012
By Richard Jefferys
In previous years, this section of the Pipeline Report has lamented the absence of any approved products in the areas that it covers. In 2012, that may finally be about to change: on May 10, the U.S. Food and Drug Administration (FDA) held a marathon 12.5-hour Antiviral Drugs Advisory Committee meeting to discuss the efficacy of the antiretroviral Truvada (a combination pill containing tenofovir and emtricitabine) for preexposure prophylaxis (PrEP) against HIV infection, and the majority of members voted for approval. The vote tallies were 19 to 3 in favor for men who have sex with men, 19 to 2 (with 1 abstention) for HIV-negative partners in serodiscordant couples, and 12 to 8 (with 2 abstentions) for other individuals at risk for acquiring HIV through sexual exposure. A final FDA decision is expected by September 14, 2012.
If Truvada is approved for PrEP, as expected, much work will still be required to define how best to implement the approach. An array of demonstration projects are now getting under way with the aim of assessing real-world use of the intervention among different populations at high risk for HIV acquisition. Research is also continuing to look at whether there are alternatives to continuous dosing of PrEP and whether antiretrovirals other than Truvada might have PrEP potential. Despite many outstanding questions, the approval of Truvada would represent a historic moment for the biomedical prevention field. The idea of combination prevention has been under discussion for many years, but with circumcision being the only biomedical approach with proven efficacy, options were limited. Approval of PrEP, taken together with emerging signs of efficacy with vaccines and microbicides, would alter the landscape dramatically. Combinations are already being tested in animal models,[1] and it was recently announced that from 2014 onward a single biennial HIV prevention conference will integrate the topics of vaccines, microbicides, and PrEP. Hopes of developing highly effective candidates have not been abandoned, but rather in the interim there is intense interest in assessing whether partially effective approaches can synergize in ways that increase their ability to reduce HIV infection risk.
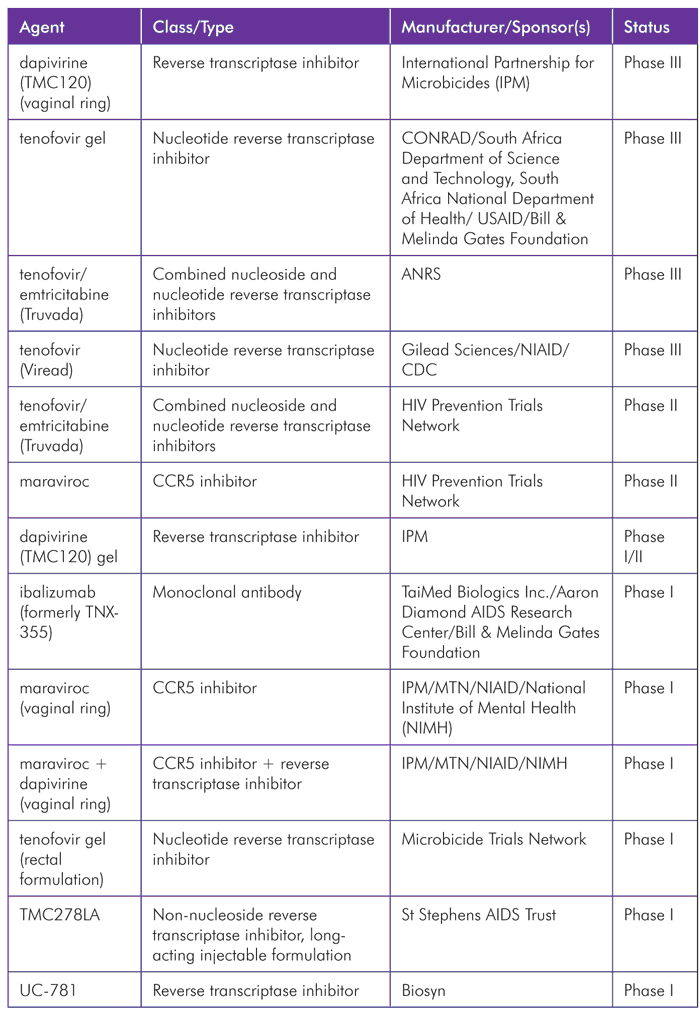
At the time the 2011 Pipeline Report was published, there was optimism that a microbicide gel form of tenofovir might be en route to licensure based on significant efficacy observed in the CAPRISA 004 trial in South Africa.[2] But news of a setback emerged on November 25, 2011, when it was announced that the tenofovir gel arm of an ongoing trial named VOICE was being discontinued due to a lack of any effect on HIV incidence.[3] The reasons for the divergent results are not yet clear, but may relate to different dosing strategies; participants in VOICE were instructed to use the gel daily, whereas in CAPRISA 004 application was within 24 hours before and after sex. Full analysis of the VOICE results will not be possible until the trial ends in August 2012. A phase III efficacy trial of tenofovir gel using the same dosing regimen as CAPRISA 004 is now taking place at nine sites in South Africa, but it is not yet known if a positive result will be sufficient to obtain approval. Although the fate of tenofovir gel is uncertain, the microbicide field has been buoyed by the recent launch of an efficacy trial of a vaginal ring that delivers the antiretroviral dapivirine; the ring needs replacing only once every four weeks, suggesting it will be considerably easier to use than prior methods. The study is sponsored by the International Partnership for Microbicides (IPM), and represents the culmination of their many years of work to develop the approach. A second complementary efficacy trial under the aegis of the Microbicide Trials Network (MTN) is due to begin within the next few months.
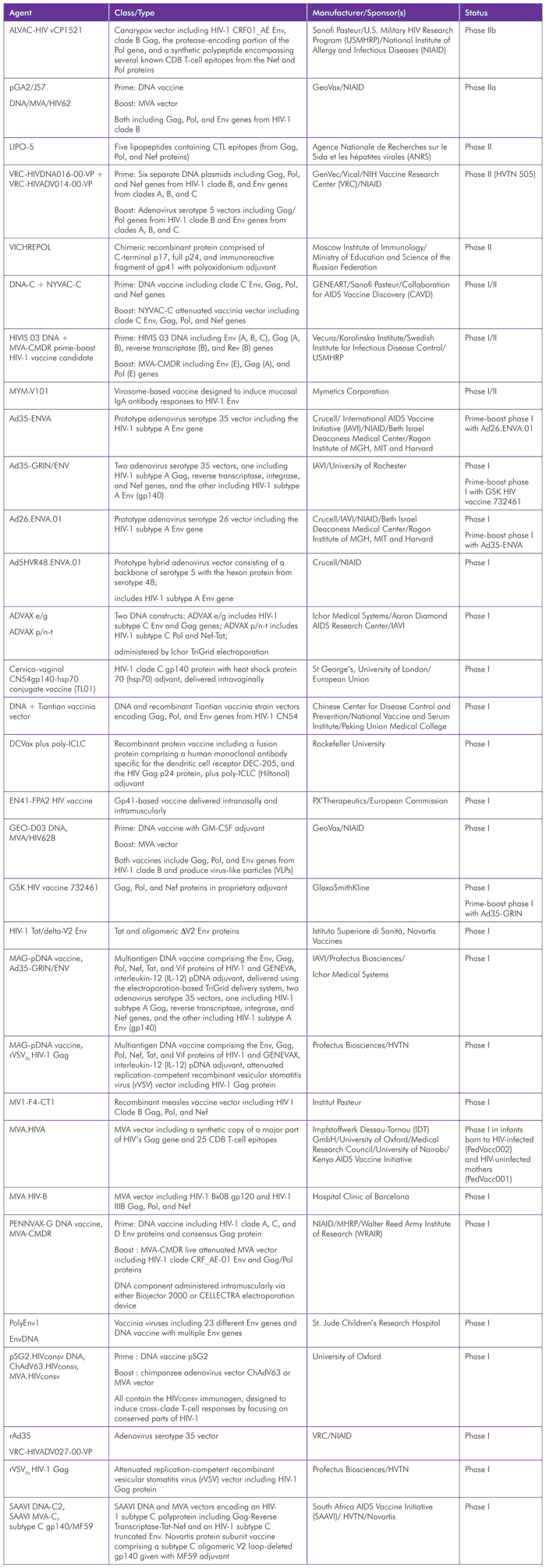
The HIV vaccine field continues to advance on multiple fronts. A key priority is following up on the marginal but significant efficacy observed in the RV144 trial in Thailand, which showed a 31% reduction in HIV acquisition associated with receipt of a prime-boost regimen comprising a canarypox vector, ALVAC-HIV vCP1521, and an envelope protein boost (AIDSVAX).[4] Over the past year, results of an analysis of possible correlates of protection have been presented and published, identifying immune responses among participants that may have been associated with vaccine efficacy.[5] Work is ongoing to better understand these findings in the hope of informing the design of new vaccines. Plans for efficacy trials of prime-boost combinations similar to those used in RV144 are well under way, with the goal of confirming and extending the results. However, these trials are not expected to open until 2014 due to delays associated with securing an envelope protein-boost component (AIDSVAX has been discontinued, and the company that manufactured it no longer exists; Novartis has been selected to produce a similar alternative).
Beyond RV144, researchers are pursuing preclinical development of novel vectors, such as those based on the virus CMV, that may be able to recapitulate the robust protection seen in animal models with live attenuated vaccine approaches (which cannot be directly translated to human use due to safety concerns). Efforts to solve the daunting challenge of inducing broadly neutralizing antibodies against HIV are progressing, but while the understanding of how to achieve broad neutralization has greatly improved, methods for creating this activity with vaccines remain elusive.
Over the past few years, investigations into curing HIV infection—once viewed as the quixotic pursuit of a few—have become a major component of therapeutic research. The shift was much in evidence at the 2012 Conference on Retroviruses and Opportunistic Infections (CROI), which for the first time featured several crowded sessions on the topic. Some signs of promise have emerged from trials of drugs that may be capable of awakening the latent HIV reservoir that has so far stymied cure efforts,[6] but perhaps the most important finding presented at CROI (and published shortly afterward in the journal Immunity) is that even if dormant HIV is successfully roused, effective immune responses against the virus are needed to deliver the coup de grace and eliminate latently infected cells.[7] Because most individuals with chronic HIV infection lack the functional T-cell responses required to accomplish this task, this study has bolstered the rationale for the use of therapeutic vaccines in cure research.
As this report was going to press, the continuing uncertainty regarding exactly how a cure is defined was thrown into sharp relief by a disheartening and unnecessary public controversy over traces of HIV genetic material that may—or may not—have been found in the lone individual widely considered to have been cured of HIV infection, Timothy Ray Brown.[8] Brown has remained off all antiretroviral therapy (ART) for five years and counting, with no signs of active HIV infection—and these are widely considered the most important criteria for a cure. Researchers are attempting to duplicate the results of Brown’s case by providing stem-cell transplants from donors homozygous for the CCR5-Delta32 mutation to additional individuals with HIV.
Immune-based and gene therapies are also being studied as possible adjuncts to ART. The goal is to address the dysregulation of the immune system that can persist in some individuals even after HIV replication is suppressed. The risk of persistent immune dysregulation increases with later initiation of ART, and features include elevated levels of immune activation and inflammation, poor CD4 T-cell increases, and an accelerated aging of the immune system referred to as immunosenescence.[9] An increasing number of studies have shown links between these phenomena and an elevated risk of morbidity and mortality,[10],[11],[12] suggesting that additional immune-based therapeutic interventions could improve the outcomes achieved with ART alone, at least in a subpopulation of people with HIV.
TABLE 1. HIV Vaccines Pipeline 2012
Correlates of HIV Infection Risk in RV144
On September 13, 2011, at the AIDS vaccine conference in Bangkok, Bart Haynes from Duke University presented the results of a massive research effort to uncover correlates of HIV infection risk in the RV144 study; the data were subsequently published in the New England Journal of Medicine.[13] Although the efficacy of the vaccines was meager over the full course of the trial, it appeared to be higher in the first year, during which there were 12 HIV infections among vaccine recipients compared to 30 in the group receiving placebo (equating to an approximately 60% reduction in risk). By identifying correlates of this apparent protection, researchers hope to find clues that will help them reproduce and maintain the levels of efficacy observed early in RV144.
Haynes led a large collaborative research effort that prioritized six different immunologic tests and then studied them in a case-control format, comparing samples from 41 vaccine recipients who became infected to 205 who did not. Samples were taken at week 26, two weeks after the final booster immunization. Multiple comparisons are involved in the analyses, and this is known to increase the possibility of obtaining statistically significant results simply by chance. The standard statistical tool for addressing this possibility is called a Bonferroni correction, but it was not used in this case because the goal was to generate hypotheses about possible immune correlates for additional studies, as opposed to confirming associations definitively. Instead of the Bonferroni method, the scientists used an approach in which each result is assigned a “q-value,” which represents the estimated chance of a false positive.
Two of the six measures showed significant associations with HIV acquisition: binding of IgA antibodies in plasma to HIV Env, which was linked to an increased relative risk of HIV infection of 1.54 (P = 0.027); in other words, vaccine recipients displaying this response at week 26 of the trial were 54% more likely to subsequently become infected than those without it. Conversely, the presence of binding IgG antibodies to the V1/V2 loops of HIV Env scaffolded onto the MLV gp70 protein was associated with a relative risk of 0.57 (P = 0.015), indicating that vaccine recipients who showed this response at week 26 were 43% less likely to acquire HIV than those who did not. For both results, the q value was 0.08, meaning that there is an approximately 8% chance they were false positives. The analyses were repeated and confirmed by a second, independent group of statisticians. Importantly, the presence of IgA antibodies to Env did not enhance HIV infection risk compared to placebo recipients; rather, vaccinated individuals with high levels of these responses experienced the same risk of infection as the unvaccinated group. The opposite pattern was true for binding IgG antibodies to the V1/V2 loops: compared to placebo recipients, vaccinated individuals with the highest levels of these antibodies were around 50% less likely to acquire HIV infection.
The reason that IgA antibodies to Env would be associated with reduced vaccine efficacy is not yet clear, but it has been suggested that these antibodies interfere with antibody-dependent cellular cytotoxicity (ADCC), one of the immunologic mechanisms that could have been responsible for the protection observed in the trial. Similarly, it is not yet known whether the binding IgG antibodies to the V1/V2 loops were directly responsible for protecting against HIV infection (whether via ADCC or some other mechanism). However, these responses did wane significantly in vaccine recipients over the six months after the final week-24 immunizations, which appears to track with the protective effect of vaccination’s being almost entirely concentrated in the first year of the trial.[14]
In separately published reports, RV144 researchers also identified the V2 region of HIV as a preferential target for vaccine-induced CD4 T-cell responses[15] and noted that certain class II HLA alleles were associated with a failure to mount antibody responses after vaccination.[16]
While much work remains, the new results represent potentially crucial clues for researchers working to improve on the marginal effect observed in RV144. Most optimistically, they hint that it might be possible to push the efficacy threshold of similar vaccine regimens over 50% by fine-tuning the types of immune responses that are induced. Although the induction of broadly neutralizing antibodies against HIV is still thought to be necessary to achieve a highly efficacious vaccine, the development of a candidate offering greater than 50% protection would be a huge step forward.
Replicating and Extending the RV144 Results
A variety of trials are under way or planned that should shed additional light on whether the RV144 results can be duplicated and improved upon. The U.S. HIV Military Research Program (USMHRP), one of the primary sponsors of RV144, is conducting follow-up trials involving ALVAC-HIV vCP1521 and the limited supplies of AIDSVAX that are still available. The RV305 trial is administering a “late boost” with ALVAC-HIV vCP1521, AIDSVAX, or both to volunteers from RV144 who received the full regimen in the original trial. Two additional smaller studies are slated to start soon; the primary goal is to investigate the immune responses induced by the vaccines—particularly mucosal responses—in greater detail than was possible with the samples available from RV144. Longer term, the USMHRP has mapped out two potential phase IIb licensure trials for the prime-boost combination of ALVAC and a gp120 protein boost, one in high-risk men who have sex with men (MSM) in Thailand, and the other among high-risk heterosexuals in South Africa.[17]
During the past year, the HIV Vaccine Trials Network (HVTN) has begun phase I evaluations of DNA and poxvirus vectors developed by the South African AIDS Vaccine Initiative (SAAVI), combined with an HIV subtype C gp140 envelope protein booster manufactured by Novartis, a first step toward the type of regimens that will be used in phase IIb efficacy trials in South Africa which, if all goes well, will be launched in 2014. Sanofi Pasteur is manufacturing a subtype C–based ALVAC vector for these trials while Novartis is in the closing stages of developing the bivalent subtype C gp120 protein boost. The HVTN has outlined the novel adaptive design that will be employed;[18] the goal is to rapidly eliminate candidates and combinations that fail to show evidence of efficacy, and prioritize those that do.
There is one ongoing HIV vaccine efficacy trial, HVTN 505, which involves a prime-boost regimen comprising a DNA vaccine followed by an adenovirus serotype 5 (Ad5) vector. The study population is circumcised MSM and male-to-female (MTF) transgender persons who lack detectable antibody responses to Ad5 (the natural form of the virus is common in nature, so some individuals have preexisting antibody responses against it). Until recently, the primary goal was to look at whether the vaccines reduced viral load in recipients who subsequently acquired HIV, but in August 2011, it was announced that in light of the RV144 results, HVTN 505 is being expanded in size from 1,500 to 2,200 participants so that the effect of vaccination on risk of HIV acquisition can also be evaluated.[19] As of May 30, 2012, the enrollment total was reported to be 1,845.[20]
The Adenoviral Odyssey
In September 2007, the HIV vaccine field received an unexpected setback when it was announced that the phase IIb efficacy trial of a candidate developed by Merck was being stopped early due to lack of efficacy. The trial was conducted by the HVTN and was referred to as the STEP study. The Merck vaccine aimed to stimulate T-cell immunity against HIV, and used a novel attenuated Ad5 vector to deliver the HIV proteins Gag, Pol, and Nef. The adenovirus-based approach was selected because it induced unprecedented levels of CD8 T-cell responses in phase I and II trials, with >70–80% of recipients responding (the previous best was 20–30% of recipients showing low-level CD8 T-cell responses after immunization with an ALVAC vector). Although HIV-specific CD8 T-cell responses were not anticipated to protect against acquisition of HIV infection, evidence indicated that they might be able to suppress HIV replication and thereby increase the chances of vaccine recipients becoming elite controllers if they became HIV-infected.
The STEP study was stopped after an interim analysis by the Data and Safety Monitoring Board (DSMB) revealed that this hoped-for salutary outcome was not being observed. Furthermore, it transpired that certain subgroups of the trial population experienced a significantly increased risk of HIV acquisition associated with receipt of the vaccine. In the overall results, this finding represented a strong trend that did not quite reach statistical significance. However, in a prespecified analysis that evaluated results based on baseline levels of antibodies to Ad5, there was a stepwise increase in the risk associated with vaccination as anti-Ad5 antibody titers increased, strongly suggesting a real biological effect. Subsequent post hoc studies revealed that the effect appeared entirely concentrated among uncircumcised MSM. To their great credit, the HVTN engaged in a massive and extremely transparent effort to investigate this outcome, involving both investigators affiliated with the network and the solicitation of input from external scientists with relevant expertise.[21]
In the time since, a variety of investigations have been conducted, but so far no causative mechanism has been identified to explain the STEP results. Unfortunately, along the way, some figures in leadership roles in the HIV vaccine field mistakenly attempted to suggest that the adenovirus vector had been absolved of having any role in enhancing HIV acquisition risk. For example, in 2009, Alan Bernstein (then head of the Global HIV Vaccine Enterprise) had this to say to the Scientist:[22]
“[This] result really rules out the possibility that it was the vaccine itself, and the fact that we used Adeno5, that was somehow increasing susceptibility to acquiring [HIV] in those volunteers.”
In 2012, two papers on the STEP trial have been published that highlight the erroneousness of Bernstein’s claim and the continuing uncertainty regarding the safety of adenovirus-based vectors. In an analysis published in the Journal of AIDS, researchers from the HVTN and Merck reported that no potential confounder could account for the increased risk of HIV acquisition associated with receipt of the Ad5 vector among uncircumcised men who have sex with men.[23] A separate report in the Journal of Infectious Diseases revealed that when assessed across the full course of the trial, the enhancement effect associated with the vaccine was statistically significant, but waned with increasing time since the last immunization.[24] Importantly, the results confirmed that no enhanced risk of HIV infection was seen at any time among circumcised individuals who lacked antibodies to Ad5 at baseline (the population being recruited for the HVTN 505 trial).
The most commonly cited hypothesis to explain the STEP outcome was that the vaccine boosted numbers of Ad5-specific CD4 T cells, thereby increasing the pool of cells potentially susceptible to HIV. But several papers have reported data that are inconsistent with this idea: blood levels of Ad5-specific CD4 T cells did not associate with acquisition risk,[25] and these responses were also rapidly induced in study participants who lacked anti-Ad5 antibodies at baseline (yet these participants experienced no increase in risk).[26] Another notion was that perhaps anti-Ad5 antibody levels correlate with HIV risk for unknown reasons, but an analysis of the Multicenter AIDS Cohort Study (MACS) did not find an association,[27] and this finding was echoed when researchers investigated the question using samples from several HIV vaccine trials.[28]
Studies have also proposed the possibility that the increased susceptibility is related to trafficking of Ad5-specific CD4 T cells to mucosal sites where adenovirus antigens are expressed,[29] but this has yet to be thoroughly explored in humans. Two macaque experiments have produced data that argue against the theory,[30],[31] but some uncertainty remains because these animals are not naturally infected with Ad5.
Continued efforts to understand the mechanism of enhancement in the STEP trial are important, because while Merck’s Ad5-based HIV vaccine has been discontinued, adenovirus vectors from an array of different serotypes—including several from chimpanzees—continue to be studied as potential vaccines against HIV, TB, malaria, and hepatitis C, and it is currently unclear if they might also have the potential to increase HIV acquisition risk.
Another recent wrinkle in the adenovirus vector story is a published study indicating that preexisting adenovirus-specific CD4 T-cell responses—which, like antibodies, are also common due to natural exposure—can impair the generation of immune responses to antigens contained in adenovirus-based vaccines.[32] Unlike antibodies, CD4 T cells cross-react with multiple human and chimpanzee adenovirus serotypes, raising the fear that these responses could impact the effectiveness of many candidates. Among the variants currently in trials are Ad35 and Ad26, which have produced promising results in the SIV/macaque model,[33] and two chimpanzee serotypes: ChAd63 and ChAd3.[34] Encouragingly, a phase I evaluation of ChAd63 as a potential malaria vaccine found that preexisting immunity to adenovirus did not appear to hamper the development of strong immune responses to the vector-encoded malaria antigens.[35]
Passive Immunization with Broadly Neutralizing Antibodies
An increasing number of antibodies capable of broadly neutralizing many different HIV variants are being identified. Among the most notable is VRC01, which potently inhibits around 90% of a panel of diverse viral isolates.[36] The future plans of the HVTN include studies that will deliver the broadly neutralizing antibodies to individuals at risk for HIV acquisition by infusion, an approach called passive immunization. Under a program launched in 2006 by the Bill & Melinda Gates Foundation called the Collaboration for AIDS Vaccine Discovery (CAVD), Gary Nabel from the Vaccine Research Center at the National Institutes of Health (NIH) was recently awarded a grant of US$1.9 million over three years specifically to develop a formulation of VRC01 to use in passive immunization studies. The primary goal is to assess whether protection can be achieved and gain an understanding of the antibody levels that might be required. One setting that is under consideration for these trials is prevention of mother-to-child transmission (PMTCT), but there are some researchers who feel strongly that this type of experiment cannot be ethically justified because, when properly implemented, antiretroviral therapy is highly effective at preventing PMTCT.[37] Others argue that there is some residual risk of transmission that could potentially be addressed by passive immunization.[38] Before these trials proceed, it will be important for there to be a broad public discussion of the issues involved. Although it would be advantageous to learn more about the protective efficacy of broadly neutralizing antibodies, methods for inducing similar antibodies with vaccines have yet to be discovered. Unless passive immunization could be made widely available—which seems an unlikely prospect given both the inconvenience of the delivery method and the cost—the potential for the populations targeted for these proposed trials to gain benefit from their participation will need to be carefully considered.
TABLE 2. PrEP and Microbicides Pipeline 2012
Preexposure Prophylaxis (PrEP)
The May 10, 2012, FDA Antiviral Drugs Advisory Committee meeting reviewed the available data on Truvada for PrEP at extraordinary length, and a webcast of the entire proceedings can be viewed online.[39] FDA briefing documents[40] and all the slide presentations from the meeting are also available.[41] The committee pored over the results of multiple trials; the two providing evidence of efficacy were iPrEx, conducted among 2,470 MSM and 29 transgender women at high risk of HIV infection, and Partners PrEP, which recruited 4,758 serodiscordant heterosexual couples. In the former trial, overall efficacy was 42% (95% confidence interval, 18–60%);[42] in the latter it was 75% (95%CI, 55–87%).[43] Adherence emerged as a key variable, with estimated efficacy being far higher among individuals with measurable drug levels: in a substudy of iPrEx, the estimated relative reduction in risk was 87.5% (95%CI, 66–95%) compared with placebo recipients;[44] in Partners PrEP it was 90% (95%CI, 58–98%).[45]
Additional studies considered by the FDA included the CDC TDF2 trial in 1,219 men and women in Botswana, in which there were a total of 33 HIV infections during follow-up: 9 among the individuals in the Truvada group and 24 among those assigned to placebo. The relative reduction in risk of HIV acquisition was 62% (95%CI, 21–83%).[46] The one trial that did not find evidence of protective efficacy was FEM-PrEP, which had enrolled 2,120 women in Kenya, Malawi, South Africa, and Tanzania when it was stopped by the DSMB in April 2011 because 56 infections had occurred: 33 in the Truvada arm, and 35 in placebo recipients. The reason for the lack of an effect is not fully clear, but it appears likely that adherence played a role; plasma drug levels were detectable in less than 50% of the Truvada recipients analyzed.[47]
Safety information for the FDA review came from the above-referenced trials and two other phase II studies of tenofovir alone that did not measure efficacy: CDC 4323, conducted in U.S. MSM, and FHI PrEP, which enrolled African women. Overall, no toxicities were identified that have not previously been documented in the context of Truvada’s approved use as an HIV treatment. The primary concerns with the drug are kidney toxicity and decreased bone mineral density (BMD). No serious kidney toxicity occurred in any trial. There were seven discontinuations of Truvada in iPrEx due to elevated creatinine; all but one of the individuals restarted without recurrence. Two Truvada recipients in Partners PrEP discontinued due to decreased creatinine clearance that resolved after the drug was stopped. A BMD decrease of greater than 5% was documented in 14% of iPrEx participants assigned to Truvada compared to 6% on placebo. A small but significant decrease in BMD also occurred among tenofovir recipients in the CDC 4323 study in comparison to those receiving placebo, and there were more reports of new onset back pain (13% vs. 6%). There were no significant differences in the incidence of new onset back pain in Partners PrEP. The occurrence of bone fractures did not differ significantly among groups in any study.
In terms of other adverse events that showed significant differences versus placebo, iPrEx reported nausea and unintended weight loss, while Partners PrEP found neutropenia occurred more frequently. Because Truvada is active against hepatitis B (HBV), one concern is that people with HBV who use PrEP might experience a flare in disease after the drug is stopped. There were 16 individuals with chronic or acute HBV in iPrEx, but no evidence of flares. Hepatic safety issues were also not seen among women with chronic HBV infection in the FHI PrEP trial.
Behavioral disinhibition or risk compensation—the idea that people might engage in activities that increase their risk of HIV infection as a result of receiving a prevention intervention—is a frequently cited bugbear in discussions about PrEP. It was not seen in any of the trials. The potential for individuals on PrEP to develop resistance to Truvada is another concern. In iPrEx, two individuals in the Truvada arm had undetected acute HIV infection at enrollment and developed resistance mutations (M184V and M184I) during the first four weeks of the trial. None of the participants who seroconverted during the trial showed evidence of drug resistance. Results were similar in Partners PrEP: three individuals in the Truvada arm had undiagnosed acute HIV infection at baseline, and one developed the M184V mutation by week 12. None of the individuals who became infected during the trial displayed drug resistance.
After reviewing the data, the Antiviral Drugs Advisory Committee delivered their votes, strongly supporting approval of Truvada for MSM and serodiscordant couples, while rendering a more equivocal verdict on the broader population of people at risk for HIV infection. The FDA’s decision on whether to approve a prevention indication for Truvada is due to be announced by September 14, 2012. The decision has been delayed by negotiations between the FDA and the manufacturer, Gilead Sciences, regarding what is called a Risk Evaluation and Mitigation Strategy (REMS) that will be required to accompany prescriptions of the drug for prevention. A REMS can comprise multiple components, such as educational guides and health care provider training plans, intended to ensure that the drug is used correctly.
In anticipation of approval, multiple demonstration projects in different populations at high risk of HIV infection are in the beginning stages. Researchers are also considering the potential impact of PrEP on trials of other biomedical preventions: the HVTN and the Microbicide Trials Network (MTN) are to launch a joint study that will evaluate the potential interactions between a DNA/NYVAC prime-boost vaccine and oral or topical PrEP.[48]
One new PrEP agent that is entering a clinical trial—jointly sponsored by the HIV Prevention Trials Network (HPTN) and the AIDS Clinical Trials Group (ACTG)—is the CCR5 inhibitor maraviroc.[49] The study intends to enroll 400 HIV-negative MSM along with a cohort of 200 women, and will primarily assess safety and tolerability of maraviroc, given alone or in combination with emtricitabine or tenofovir.
Two trials are exploring intermittent use of PrEP. The HPTN is conducting the ADAPT study (Alternative Dosing to Augment PrEP Tablet-Taking, also known as HPTN 067) which is comparing different Truvada dosing schemes in 180 MSM and 180 heterosexual women at high risk of acquiring HIV infection. The trial is not of sufficient size to evaluate efficacy, but will assess tolerance, acceptability, and drug levels. In France, the ANRS is sponsoring IPERGAY, which is recruiting 300 MSM for an initial pilot phase. The schema involves taking two doses of Truvada (or placebo) within 24 hours prior to sexual activity, one dose every 24 hours during the period of sexual activity, and one dose 24 hours afterward. Depending on the results of the pilot phase, the trial may expand to enroll an additional 1,600 MSM.[50]
Microbicides
The major news in the microbicide field is the recent launch of The Ring Study (also known as IPM 027), a large phase III efficacy trial of the antiretroviral dapivirine, delivered via a vaginal ring. A total of 1,650 women will be enrolled at sites in South Africa, Rwanda, and Malawi. Developed and sponsored by the IPM, the dapivirine ring delivers drug for a four-week period before it needs replacing, potentially providing women with a convenient and discrete prevention method that is entirely under their control. A second complementary phase III trial of the approach, sponsored by the MTN and named the ASPIRE study, is due to start soon. ASPIRE will recruit 3,476 women from sites in Malawi, South Africa, Uganda, Zambia, and Zimbabwe.
The IPM has received funding from USAID to further develop the dapivirine ring with the aim of creating a modified version that can deliver drug for 60 days in combination with a contraceptive. Rings that deliver maraviroc alone or combined with dapivirine are also being studied in phase I trials.
Tenofovir gel, which reduced risk of HIV acquisition by 39% in the CAPRISA 004 study, is now being tested again in South Africa in a larger efficacy trial named FACTS 001. The goal is to enroll at least 2,200 women and obtain a definitive answer as to whether the approach works. A rectal formulation of tenofovir gel is also in development, after a safety study evaluating rectal application of the vaginal version revealed that it caused a surfeit of unpleasant gastrointestinal side effects.[51] Early results with the rectal formulation suggest it is far better tolerated,[52] and additional trials are imminent.
TABLE 3. Research Toward a Cure 2012
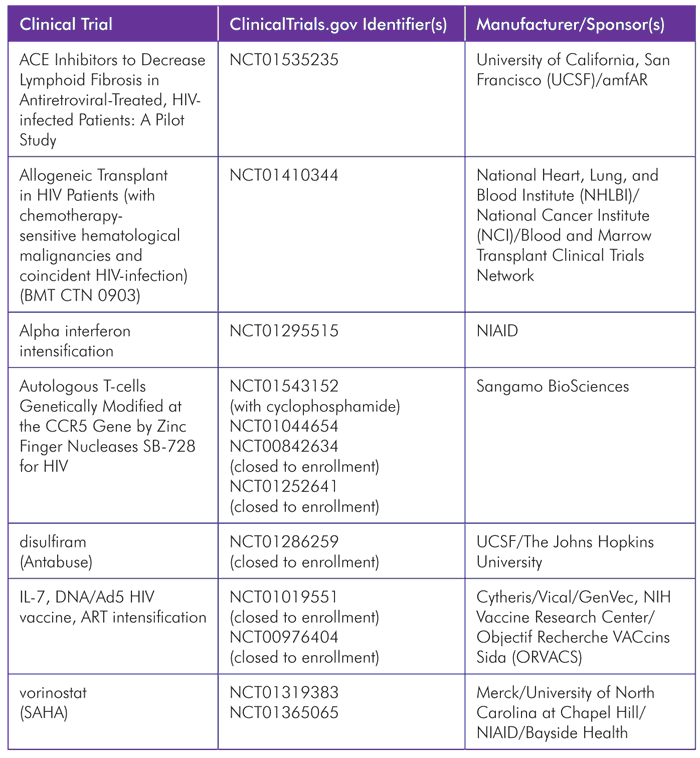
Cure research has become increasingly high-profile over the past year, but relatively few new clinical trials have been initiated. When evaluating the research portfolio, however, it is important to appreciate that the field is awash in definitional uncertainty. For example, the recent evidence suggesting therapeutic HIV vaccines have an important role to play means that, technically, all studies of these approaches could be considered cure research. Certainly, manufacturers of therapeutic vaccines have been quick to cite the goal of achieving a functional cure—control of HIV replication in the absence of ART—as pertinent to their products. For the purposes of this section of the Pipeline, we have focused on trials that make specific reference to assessing the impact of an intervention on the latent HIV reservoir, or that are connected to the CCR5 abrogation strategy that appears to have been central to the cure achieved in Timothy Brown.
New studies include an evaluation of whether angiotensin converting enzyme (ACE) inhibitors can reduce scarring damage to the lymph nodes (fibrosis) in HIV infection, and thereby also reduce the HIV reservoir. Lymph node fibrosis has been shown to progressively worsen during untreated HIV infection,[53] and can persist and limit CD4 T-cell recovery after ART initiation.[54]
Under the leadership of Richard Ambinder at the Johns Hopkins University and Joseph Alvarnas at the City of Hope National Medical Center, the Blood and Marrow Transplant Clinical Trials Network has opened a trial for HIV-positive individuals with chemotherapy-sensitive hematologic malignancies that will attempt to identify stem cell transplant donors homozygous for the CCR5-Delta32 mutation. The goal is to try to duplicate the results obtained in Timothy Brown. A company named StemCyte is pursuing the same goal with a slightly different approach: stem cell transplants derived from cord blood. At a recent conference, Lawrence Getz from StemCyte reported that so far they have identified around 102 cord blood donors homozygous for CCR5-Delta32 out of around 17,000 tested. Although there is no formal trial, an individual with HIV in the Netherlands has recently received such a transplant as part of treatment for a hematologic malignancy, and the same procedure is about to be used in a similar case in Madrid.[55]
By pairing zinc finger proteins with enzymes called nucleases that can break up DNA, the experimental therapy being developed by Sangamo BioSciences—SB-728—disrupts the CCR5 gene and thus prevents expression of the CCR5 coreceptor on modified cells. In current trials, CD4 T cells are extracted from participants via apheresis, subjected to the zinc finger nuclease procedure in the laboratory, and then expanded in number and reinfused. Early trial results were available last year, but there have been several developments since that time.
Most intriguingly, one study involves a 12-week interruption of ART, and participants have shown evidence of viral load declines prior to ART reinitiation. Analyses of the data revealed a significant inverse correlation between the number of detectable gene-modified CD4 T cells and viral-load levels, indicating an antiviral effect.[56] One notable individual showed a viral-load reduction to undetectable levels prior to restarting ART, and it turned out that this person was heterozygous for the CCR5-Delta32 mutation; because this renders one of the two CCR5 genes present in each cell defective, there was less work for Sangamo’s therapy to do, and the levels of modified cells were much higher. In an attempt to duplicate and extend these findings, Sangamo is now specifically recruiting individuals heterozygous for CCR5-Delta32 into an expanded trial. Another new study is evaluating whether a brief period of immune-suppressive treatment with the drug cyclophosphamide can increase the expansion of gene-modified CD4 T cells after infusion (essentially by making more “space” for them to flourish).
The leading strategy for awakening the latent HIV reservoir involves the use of a class of anticancer drugs called histone deacetylase (HDAC) inhibitors. Numerous in vitro studies have shown that these drugs can stimulate HIV RNA expression by latently infected CD4 T cells.[57] Toward the end of 2011, David Margolis from the University of North Carolina presented the first human data on the approach, and he delivered further updates at the 2012 CROI[58] and Keystone[59] meetings.
Margolis is conducting a phase I/II trial of the HDAC inhibitor vorinostat (also known as SAHA, trade name Zolinza) in people with HIV on long-term ART with suppressed viral loads. The protocol schema is complex, partly due to safety concerns. The anti-latency effect of the drug is being measured 4–6 hours after a single 400 mg dose. Because latently infected CD4 T cells are very rare, large numbers of cells (approximately 4 billion) are extracted from each participant at baseline and after receipt of the drug. The samples are divided into pools of around 1 million purified resting CD4 T cells each, ending up with 24–36 pools per person at each time point. HIV RNA expression is then measured in each pool, and averaged to arrive at a median level for each individual, before and after vorinostat treatment. At the Keystone conference, Margolis was able to report results from seven participants, all of whom showed an increase of HIV RNA expression. The median increase for the entire study population compared to baseline was 5.2-fold. Margolis believes this is evidence that the drug is working as hoped.
In Australia, Sharon Lewin from Monash University is undertaking a trial of vorinostat that involves 14 days of treatment as opposed to a single dose. Data on the effect on the latent HIV reservoir are not yet available, but Lewin was able to present preliminary safety results at CROI.[60] Grade 1 and 2 adverse events were common, including lethargy, nausea, vomiting, diarrhea, thrombocytopenia (decreased platelet counts), and increased levels of the enzyme alkaline phosphatase; all resolved after the 14-day dosing period. This panoply of side effects is consistent with what is known from the use of vorinostat in cancer, and illustrates why HDAC inhibitors are being considered only for short-term use in cure-related research.
An important question pertaining to latency-reversing approaches is whether successful induction of HIV RNA expression in latently infected CD4 T cells will be sufficient to cause cell death. Two studies debuted in 2012 suggest that the answer to this question is no. The laboratory of Tae-Wook Chun at NIAID explored the issue using in vitro assays and found that HDAC inhibitors did not cause latently infected CD4 T cells to die by virus-induced cytopathic effects.[61] Liang Shan from Robert Siliciano’s research group at the Johns Hopkins University obtained similar results but found that, after exposure to HDAC inhibitors, the CD4 T cells could be eliminated by functional HIV-specific CD8 T cells. However, while HIV-specific CD8 T cells sampled from elite controllers performed this task with gusto, the same was not true for most individuals with chronic infection. In order to persuade HIV-specific CD8 T cells from the latter group to work, they needed to be stimulated with HIV antigens prior to being mixed with the latently infected cells. Shan and colleagues conclude that therapeutic HIV vaccines will need to be combined with anti-latency strategies if elimination of the latent reservoir is to be achieved.[62]
Disulfiram (Antabuse) is an approved drug used to treat alcoholism that has shown anti-latency potential in a laboratory study.[63] Preliminary results of a small phase I trial were presented at the 2012 CROI but did not provide clear evidence of an effect.[64] There was a suggestion of an increase in HIV RNA expression very soon after dosing; additional work is now being performed to assess whether this observation was real or artefactual.
On the cure-research funding front, in July 2011 NIAID announced the award of three multimillion-dollar five-year grants under the aegis of the Martin Delaney Collaboratory, a program named in memory of the longtime AIDS activist and founder of Project Inform, who died in 2009. Grantees include:
- David Margolis at the University of North Carolina at Chapel Hill, who is leading the largest of the groups, consisting of 15 scientific projects at nine different academic research centers throughout the U.S. Merck Research Laboratories is a key part of this team, but will not be receiving funding from the National Institutes of Health (NIH). The major goals are to improve the understanding of HIV persistence despite antiretroviral therapy and to develop therapies to target and eliminate viral reservoirs.
- A triumvirate of principal investigators—Steve Deeks and Mike McCune at University of California, San Francisco, and Rafick-Pierre Sékaly at the Vaccine and Gene Therapy Institute of Florida—who are overseeing seven projects aiming at determining where HIV reservoirs are located in the body and how they are created and maintained, with the ultimate goal of developing therapies that can eliminate reservoirs without causing excessive immune activation.
- Keith R. Jerome and Hans-Peter Kiem at the Fred Hutchinson Cancer Research Center, who are embarking on five projects, including a collaboration with Sangamo BioSciences on the use of hematopoietic cell transplants to create HIV-resistant immune cells (Kiem has developed a macaque model for evaluating this type of approach). Jerome is also pursuing the use of proteins called endonucleases to excise the HIV genome from latently infected cells.[65]
A glimpse at Hans-Peter Kiem’s preclinical work was offered earlier this year when he presented results of a small macaque experiment that introduced a gene encoding an anti-HIV fusion inhibitor into stem cells and transplanted them into the animals, giving rise to a population of CD4 T cells resistant to infection.[66] Although only a minority of the total CD4 T-cell population displayed evidence of gene modification, the macaques exerted an unusual degree of control over a SHIV challenge and did not progress to simian AIDS. The researchers believe that gene-modified virus-specific CD4 T cells likely mediated the effect. In future experiments, they plan to study whether immunization with SHIV antigens after transplantation can enhance the numbers of gene-modified virus-specific CD4 T cells and further improve control of viral replication.[67] Depending on the outcome, it may open another door for therapeutic vaccines—in this case to be used in combination with gene therapy approaches.
Defining a Cure
In addition to the uncertainty regarding exactly what constitutes cure research, a recent unfortunate outburst of controversy has highlighted the fact that there is no consensus as to exactly how a cure is defined. The situation arose after a presentation by Steven Yukl from UCSF describing the results of intensive studies searching for HIV in Timothy Brown. Almost all the results were negative, including tests for infectious virus in vast numbers of cells (approximately 9 billion). No viral RNA or DNA could be found in peripheral blood mononuclear cells (PBMCs) or cerebrospinal fluid (CSF). But trace amounts of HIV RNA were detected in plasma by two laboratories, and another laboratory obtained positive results for HIV DNA in a minority of rectal samples. Genetic sequencing results were suggestive of contamination in at least one instance (a common problem with the assays used). The researchers involved in the study were careful to note that the results do not mean that Timothy Brown isn’t cured, but rather illustrate the difficulty of formally distinguishing between a sterilizing cure—in which all virus is eradicated—and a functional cure, the term used to refer to the scenario where any residual HIV is controlled in the absence of any treatment. This did not prevent a barrage of wild speculation about the results from one scientist, and the appearance of a slew of press stories—of varying accuracy—on the subject. It is likely that researchers will be wrestling with the question of how best to define a cure for some time.
Immune-Based and Gene Therapies, and Therapeutic Vaccines
As touched on in the preceding section, the cure research renaissance has opened up new opportunities for these black sheep of the therapeutic pipeline. Until quite recently, the increasing effectiveness and tolerability of ART, along with the new appreciation of the inflammatory dangers posed by uncontrolled HIV replication, had led to a waning of interest in alternative approaches. Although most of the candidates in these categories predate the renewed interest in curing HIV, it is likely that many—particularly therapeutic vaccines—are destined to be studied in that context rather than as an adjunct to ART.
The exceptions are therapies that aim to address the immune dysfunction that can persist in some HIV-positive individuals despite suppression of viral replication. Currently, the cytokine IL-7 appears to be the only immune-based therapy with any prospect of being evaluated for clinical benefit in this setting. A new study of IL-7 presented at the 2012 CROI may bolster the case for further studies, as it found that in addition to increasing CD4 and CD8 T-cell numbers in peripheral blood, administration of the cytokine to HIV-positive individuals on ART boosted CD4 T-cell levels in the gut and reduced soluble CD14 and D-Dimer, two inflammation-associated biomarkers that have been linked to mortality.[68]
TABLE 4. Immune-Based and Gene Therapy Pipeline 2012
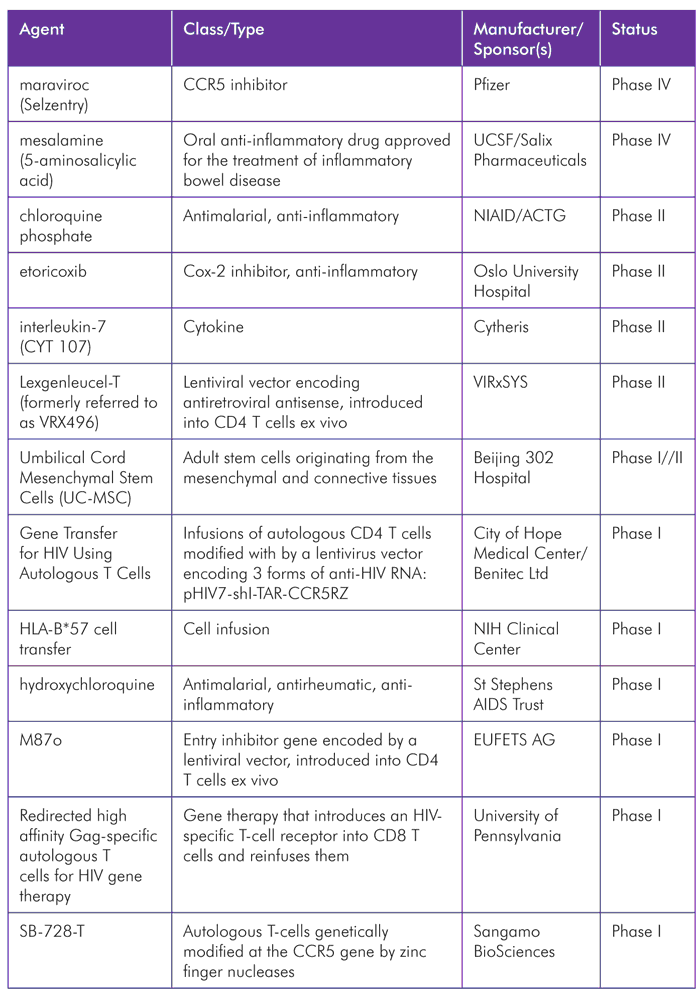
TABLE 5. Therapeutic Vaccines Pipeline 2012
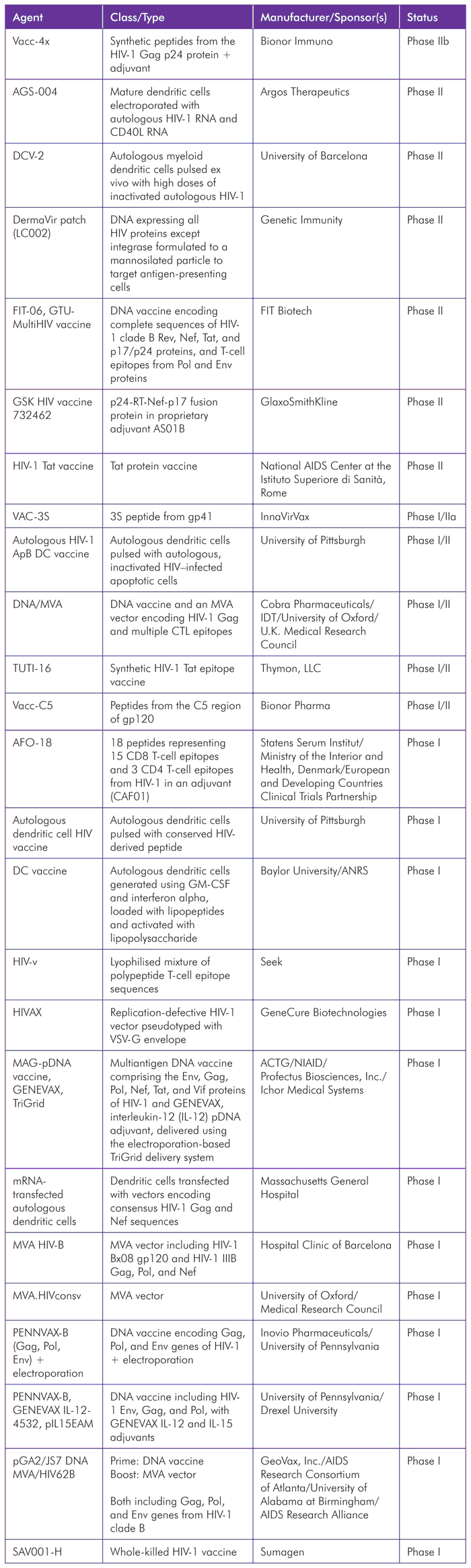
A number of developments have occurred in the therapeutic HIV vaccine field over the past year. While there have been no earth-shattering breakthroughs, two studies have added to prior hints that HIV-specific immunity can be modulated sufficiently to reduce viral load, even though the effects have generally been meager and transient. In one case, a DNA vaccine developed by FIT Biotech appeared to make a very mild dent in viral load levels among individuals for whom ART was not yet indicated.[69] A post hoc analysis from a phase II trial of Vacc-4x, a peptide-based vaccine developed by Bionor Pharma also suggested a reduction in viral load during an ART interruption.[70] While it is hard to envision these results leading to therapeutic vaccines replacing ART, they do offer reasons to hope that in cure research—where the aim is to deal with small numbers of infected cells in combination with other approaches—the enhancement in HIV-specific immunity might be able to make a crucial contribution.
There are several newcomers to the therapeutic HIV vaccine pipeline. Jonas Salk’s whole-killed candidate Remune is long gone, but a similar vaccine developed by Sumagen is entering phase I. Although they are often derided, killed vaccines can be highly effective at inducing CD4 T-cell responses, and recent data indicate that HIV-specific CD4 T cells can play an important role in controlling viral load.[71] HIVAX is an unusual contender developed by GeneCure Biotechnologies; unlike most vaccines, it is based on a nearly entire replication-defective HIV genome, meaning it encodes almost all viral antigens.
Two candidates are not designed to enhance HIV-specific immunity, but rather to induce antibody responses that may reduce the ability of the virus to cause harmful effects (such as CD4 T-cell apoptosis and immune activation). VAC-3S aims to induce antibodies against an epitope from the HIV gp41 protein, based on the idea that this will prevent CD4 T cells being nudged into apoptosis by natural killer cells.[72] Bionor Pharma is developing Vacc-C5 as a complement to their Vacc-4x construct. The vaccine is based on the C5 protein from gp120, and the rationale is that antibodies against this target may reduce immune activation.[73]
Conclusion
To the extent that a theme can be identified in the disparate pipelines covered in this chapter, it is: combine, combine, combine. The imminent arrival of PrEP is not viewed by anyone as a panacea for prevention, but rather a step toward the availability of a smorgasbord of options that can be mixed and matched for maximum convenience and effectiveness, depending on an individual’s situation. HIV vaccines have finally ditched the dichotomy of cellular versus humoral immunity and, absorbing the lessons of RV144, embraced the marriage of the two. Cure research, once viewed as the domain of monomaniacal virologists, finds itself calling for immunologic contributions from therapeutic vaccines. Hopefully, the tools we need to prevent and cure HIV infection will soon emerge from this dizzying search for synergies.
References
